Insulin 100
Celebrating a Century of Health
Innovation at the University of Toronto
Our revolutionary discovery of insulin has saved millions of lives.
It also sparked a culture of ingenuity and collaboration that continues to change the world.
A Life Saving Discovery is Born
Five-year-old Teddy Ryder was among the first patients to receive the “pancreatic extract” co-discovered by Frederick Banting and Charles Best at the University of Toronto in the summer of 1921. He would go on to live 71 more years with diabetes, one of millions of lives saved and made better by insulin.
Left to right: Teddy Ryder on the day he was given his first insulin injection. Early press coverage of insulin’s discovery.
When news of insulin’s discovery broke in the spring of 1922, Teddy’s weight had dropped to just 26 pounds. He’d lost interest in playing and was unable to take more than a few steps on his own.
Writing to Frederick Banting, Teddy’s uncle—a doctor at New York’s Bellevue Hospital—stressed his nephew’s perilous condition: “It looks to me as though a very few months … will be all he can hold out … I need not tell you how earnestly I hope you will see your way clear to treat him.”
Banting did see his way to treating Teddy. Travelling to Toronto by train with his mother, the little boy received his first dose of insulin on July 10, 1922. By the fall Teddy was strong enough to return home to his family and a new life in New Jersey. “I wish you could come to see me,” the now robust six-year-old wrote to Banting the following year. “I am a fat boy now and I feel fine. I can climb a tree.”
I am a fat boy now and I feel fine. I can climb a tree.

Insulin Belongs
to the World
Banting recorded the idea for insulin in his notebook.
The idea for insulin came to Frederick Banting in the wee hours of the morning of October 31, 1920. Waking from a fitful sleep, Banting scribbled down a 25-word hypothesis that, within the span of a year, would lead to one of the most significant medical discoveries of the 20th century.
With no lab space or research experience, Banting approached U of T physiology professor J.J.R. Macleod—an international expert in diabetes—who agreed the idea was worth testing, on the condition that Banting agree to devote all of his energies to the project.

On May 17, 1921, Banting and physiology and biochemistry student Charles Best, who’d won a coin toss to become Banting’s assistant, began their experiments under Macleod’s direction at the University of Toronto.
The pair spent the spring and summer testing Banting’s theory and by August of 1921 their notebooks were recording promising results—after repeated failures and refinements their extract was, at last, bringing down blood sugar levels.
Progress continued into the winter of 1921, when biochemistry professor James B. Collip was brought on board to purify the pancreatic extract, thereby making it safe for human trials.
On January 23, 1922, Leonard Thompson, a 14-year-old Toronto boy who was drifting in and out of consciousness at Toronto General Hospital, became the first person to receive the purified extract of what would come to be called “insulin.”

Insulin’s effect on diabetic patients was nothing short of miraculous. Bill Bigelow, a young U of T surgeon who witnessed the early insulin trials, recalled seeing comatose patients “awakened dramatically, snatched from death’s door.”
Early Insulin Patients
A discovery was born. Diabetic clinics were established at the Christie Street Veterans Hospital, Toronto General Hospital and the Hospital for Sick Children. U of T’s Connaught Antitoxin Laboratories began ramping up insulin production and the University entered into an agreement with Eli Lilly & Co. to begin large-scale production—bringing insulin from bench to bedside with revolutionary results.
A Nobel Prize in Medicine Followed
In the century since the breakthrough that historic summer of 1921, insulin has saved and improved the lives of millions of people with diabetes—here in Canada and across the globe.
Historical photographs courtesy of the Thomas Fisher Rare Book Library, University of Toronto.
Igniting a Century of Discovery
Insulin focused the eyes of the world on Toronto and established the city as the vanguard of diabetes research and treatment.
On this illustrious foundation, U of T and its hospital and industry partners built a culture of discovery, innovation and collaboration that has transformed health care and continues to have a ripple effect worldwide.
Over the past century, Toronto scientists have made game-changing advancements in biomedical sciences, human health and health care.
Banting and Best discover insulin.
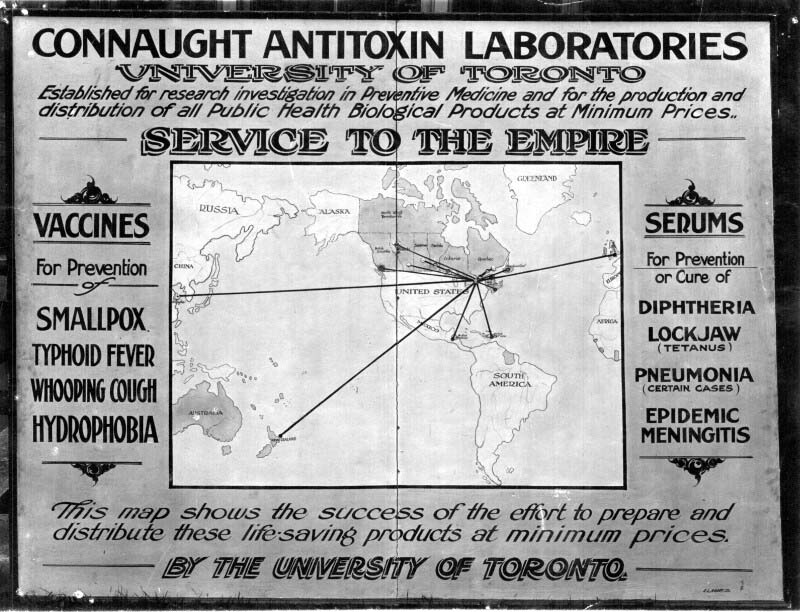
The discovery of insulin spurs considerable growth in the Connaught Laboratories and public health education, leading to the creation of the School of Hygiene. The School is the third of its kind in North America after Johns Hopkins and Harvard.
A research team at Connaught, led by Charles Best, develops a method to purify heparin, which makes the drug safe for human use and opens the door to such operations as organ transplants and open-heart surgery.
John Ross’s studies of lead poisoning in children result in the prohibition of lead pigments in paints for children’s toys and furniture.

Norman Bethune organizes the first mobile blood transfusion unit.

Leone Farrell develops what comes to be called the “Toronto Method,” later adapted to cultivate the poliovirus on a large scale for vaccine production, involving bottles that were gently rocked on a custom designed machine.
Raymond Parker’s research with viruses and cancer cell nutrition leads to developing the world’s first purely synthetic medium to support tissue culture studies, known as “Medium 199.”

Wilfred G. Bigelow develops the first electronic heart pacemaker.
Considered the fathers of stem cell science, James Till and Ernest McCulloch discover the hemopoietic (blood forming) stem cell at Princess Margaret Hospital, which becomes the basis for regenerative medicine.
W. T. Mustard perfects his surgical method for correcting “blue baby” syndrome.
Phil Seeman discovers the dopamine D2 receptor, which transformed antipsychotic drug design.

Vera Peters revolutionizes the way we approach cancer treatment by showing that treating early-stage breast cancer with lumpectomy and radiation is just as effective as radical mastectomy.

David Jenkins develops the Glycemic Index, revolutionizing how we eat.
Joel Cooper leads the world’s first single-lung transplant surgery.
Tak Mak helps to identify the T-cell receptor gene, a major advance in understanding the body’s immune system.
Alan Hudson and Susan Mackinnon perform the first nerve transplant.

Lap-Chee Tsui and Manuel Buchwald isolate the gene causing cystic fibrosis.
Tony Pawson leads the team that identifies how cell receptors transmit signals instructing the cell to change, leading to major advances in cancer research.
John Dick identifies cancer stem cells.
Peter St George-Hyslop leads a team that discovers two genes responsible for early-onset Alzheimer’s disease.
Daniel Drucker discovers and develops a glucagon-like peptide 2 (GLP-2) for chronic therapy for short bowel syndrome.

Brenda Gallie leads the team that develops a new therapy for retinoblastoma, signalling the first major change in the management of the disease in 35 years.
Lewis Kay develops new nuclear magnetic resonance (NMR) methodologies that become global standards in laboratories around the world and revolutionize the study of proteins.
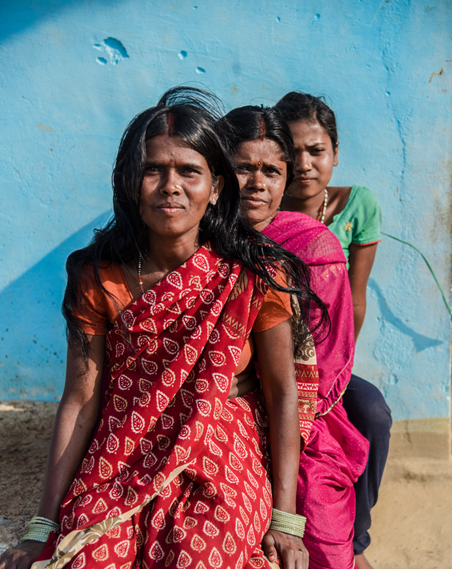
Steven Narod and colleagues identify genes responsible for familial forms of breast and ovarian cancers.
Stanley Zlotkin develops Sprinkles to add essential vitamins and minerals to baby foods in developing nations.

Stephen Scherer’s contributions to the Human Genome Project lead to a better understanding of the genetic factors underlying autism and other diseases.
Andres Lozano pioneers the technique of deep brain stimulation for surgically treating depression, Alzheimer’s disease and other disorders.

Geoffrey Hinton codevelops Deep Learning, a machine-learning paradigm that is changing how medicine is practiced.

James Dou and Stewart Aitchison develop a hand-held device for monitoring white blood cells in HIV patients who live in remote locations.

Derek van der Kooy uses stem cells to restore sight in blind mice.

Prabhat Jha launches the world’s largest public health study.
Milica Radisic becomes the first to use electrical pulses to turn stem cells into mature cardiac cells, signalling a significant advance in tissue engineering.
Todd Mainprize performs the first surgery to non-invasively penetrate the blood-brain barrier and deliver chemotherapy to a brain-tumour patient.


The Next 100 Years
Building on this century of success, the University of Toronto continues to lead revolutions in human health through an integrated approach to health research—from fundamental science through to the clinic and into the marketplace.
A collaborative culture brings together researchers across a range of domains, including regenerative and precision medicine, pharmacology and drug development, molecular medicine and the biology of disease, mind and brain health, metabolism and nutrition, and global health, public health and health systems —to name but a few of U of T’s strengths.
Here in Toronto, we have one of the world’s greatest concentrations of stem cell scientists, tissue engineers, transplant experts and brilliant researchers and clinicians in every discipline.
U of T Continues to Lead Revolutions in Human Health

Today, our scientists are developing novel therapeutic strategies to diagnose, treat and potentially cure diabetes. We are probing the link between the gut microbiome and Type 1 diabetes and working to create a renewable pool of insulin-producing beta cells for transplant into patients.

We are using Deep Learning, a game-changing artificial intelligence technique developed at U of T, to transform how doctors practice medicine and mapping a tumour’s DNA to determine the most effective therapy to treat a patient’s cancer.
Our researchers are using stem cells to cure blindness in mice, engineering tissue patches that can repair damaged hearts, and creating miniscule models of the nose, mouth, eyes and lungs to better understand why COVID-19 is so good at breaking through the body’s natural defenses.
TransformativeResearch

Our scientists are driving transformative research to better treat and ultimately prevent Alzheimer’s and Parkinson’s disease and pioneering innovative approaches to understanding the biological causes of depression.

We are optimizing diets based on our personal genetic code and engineering dietary supplements to prevent vitamin deficiencies among pregnant women, nursing mothers and young children in developing countries.
Global Reach
We are conducting one of the largest public health studies in the world in an effort to reduce the number of child deaths in India and are using machine learning to suggest ways to reduce diabetes rates in Canada—and save millions in potential health-care costs.

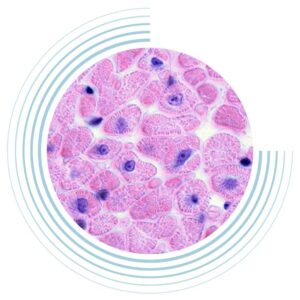
U of T scientists are discovering biomarkers that can detect disease before patients even feel sick and developing drugs and targeted treatments which offer hope to those with rare and devastating diseases.

Our researchers are working to close the health gap that makes it harder for women to access health care, receive accurate diagnoses or benefit from research on their specific risk factors.
And the legacy of excellence and innovation established by Connaught Laboratories and The School of Hygiene lives on in the scores of U of T scientists, clinicians and global health experts who are leading Ontario and Canada’s response to the COVID-19 pandemic.
A Better Tomorrow
The revolutionary discovery of insulin in 1921 ignited a century of groundbreaking research and innovation at U of T that continues to advance human health and give people around the world a chance to live up to their full potential.







While a cure for diabetes is yet to come, the Nobel Prize-winning discovery of insulin continues to save the lives of millions of people worldwide and the University of Toronto continues to be a leader in research and treatment of the disease.
In the years and decades ahead, we will keep pushing the boundaries of what’s possible, advancing the culture of ingenuity and collaboration that started a century ago with Frederick Banting, Charles Best, J.J.R. Macleod and James B. Collip.
Where Will Health Innovation Take Us Next?
U of T is grateful to its network of partners including:
Sir Frederick Banting Legacy Foundation; Banting Research Foundation; Charles H. Best Foundation; Canada Post; CIHR’s Institute of Nutrition, Metabolism and Diabetes; Defining Moments Canada; Diabetes Action Canada; Diabetes Canada; Historica Canada; Lilly Canada; JDRF; Medicine by Design; Novo Nordisk; Parks Canada; Royal Canadian Institute for Science; Sanofi Canada; Toronto Medical Historical Club; and University Hospital Network.